Claims Lack Real-Time Oversight

Claims review happens across fragmented tools

Manual workflows slow down intervention

Transparency data is disconnected from claims

Scaling review requires more headcount

Risk trends hide payment leakage

No visibility into claim decisions

Large claimant signals arrive too late

Risk priced without payment controls
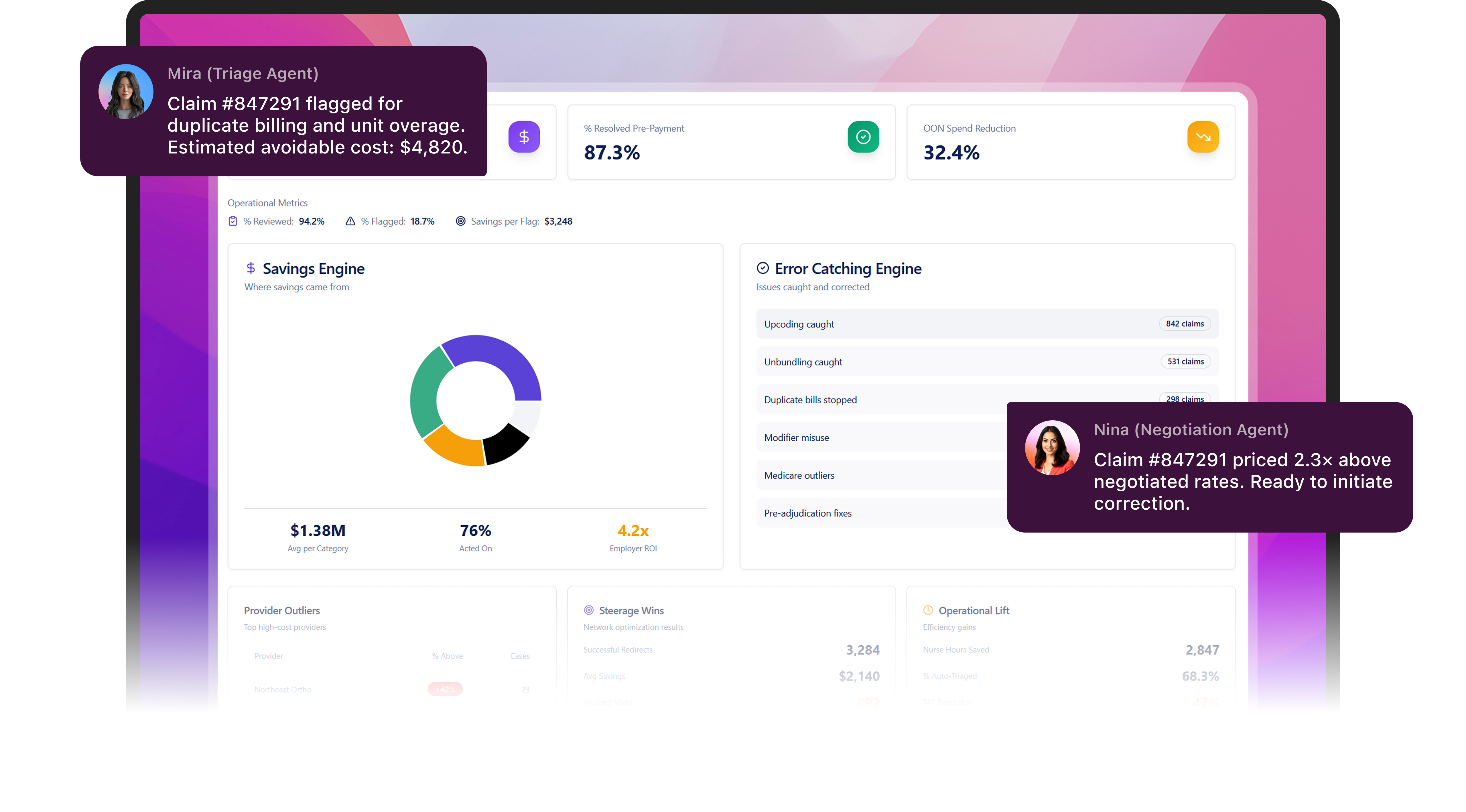
BenOsphere helps TPAs prevent up to 10% claim leakage before payment and gives Underwriters visibility into loss ratio drivers beyond clinical risk
A Claims Triage and Negotiation Platform
100% Claims Triaged
Reviews claims for pricing issues, unbundling, upcoding, and duplicate charges.
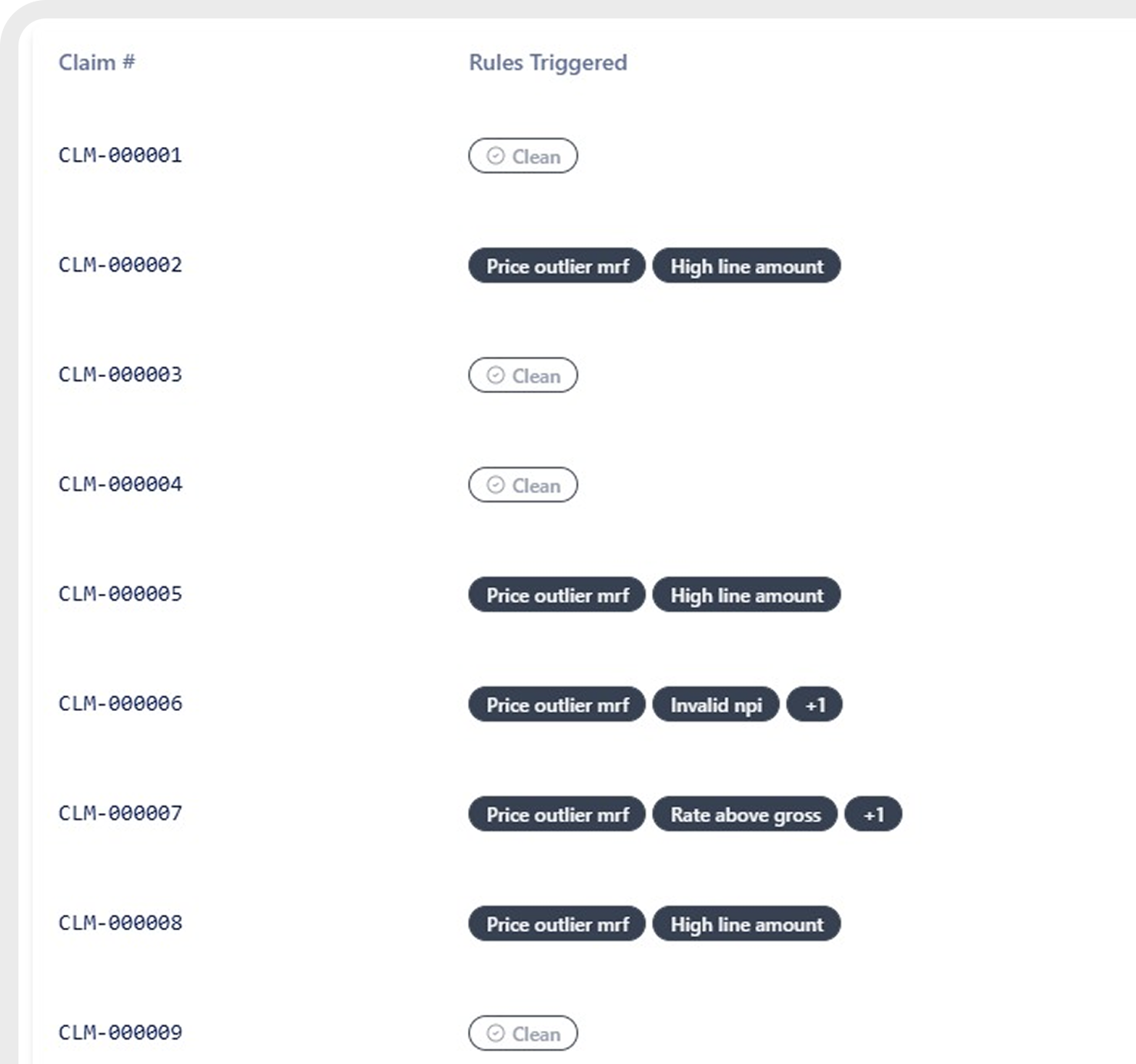
Price Transparency
Benchmarks billed amounts against payer and hospital price data.
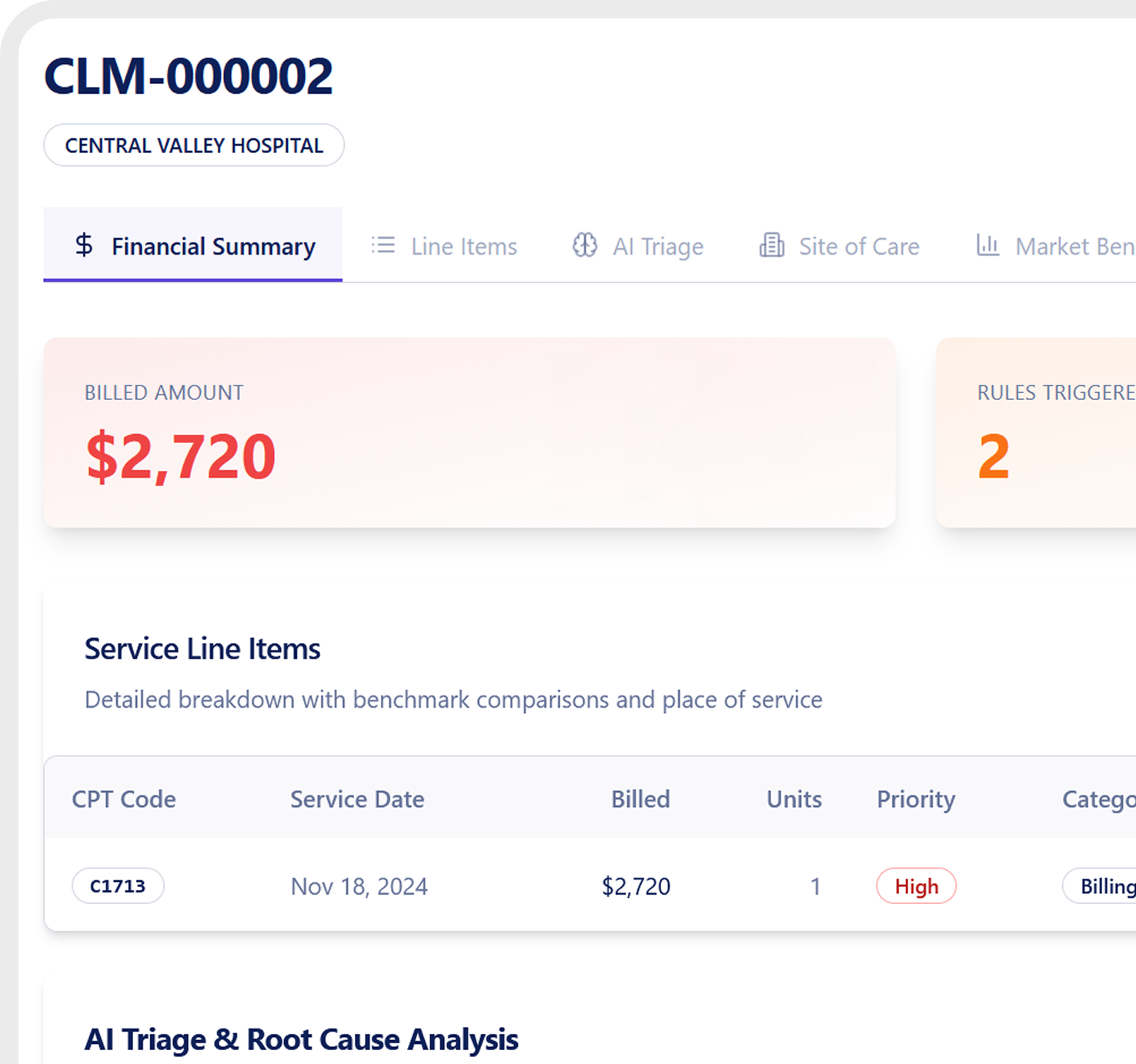
Focused Intervention
Only claims with real savings potential are routed for negotiation or action.
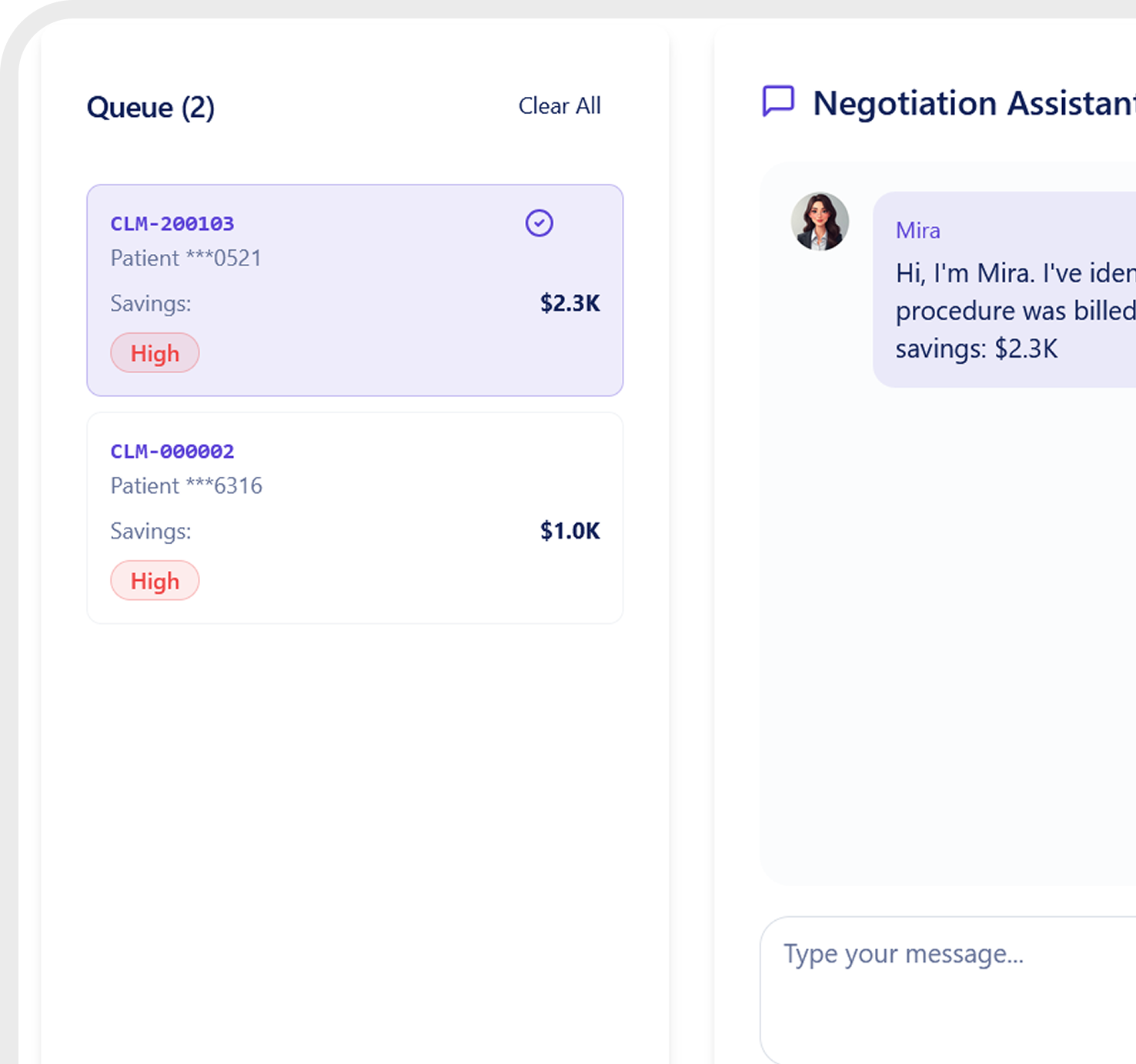
Real-Time Oversight
Gives TPAs and Underwriters live visibility into claims and payment accuracy.
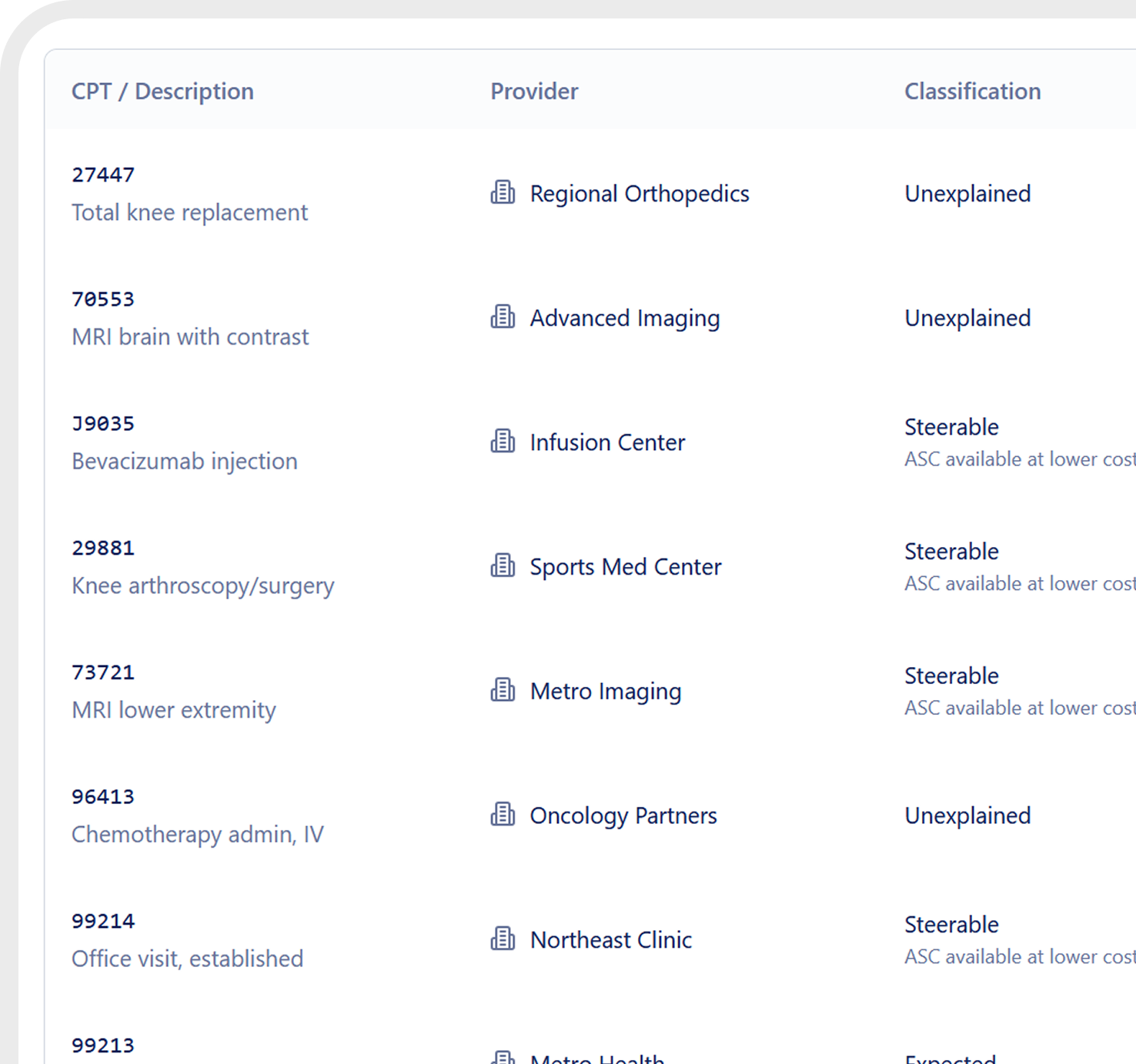
Claims Intelligence Powered by AI Agents
Every claim reviewed, triaged and documented before payment.
.png)
Mira
Reviews every claim and flags pricing errors, coding drift and billing risks.
.png)
Nina
Prepares negotiation evidence and pricing benchmarks for claim correction.

Theo
Gives Underwriters visibility into claim quality and loss ratio drivers.
Give TPAs and Underwriters Real Control Over Claims
TPA Operational Oversight
See claims as they move through the system before payment
TPA Cost Exposure Clarity
Identify where claim spend is accumulating and where intervention matters most.
Underwriter Risk Visibility
Understand what drives loss ratios before renewals and pricing decisions.
Underwriter Intelligence
Reveal claim quality signals behind loss ratios.
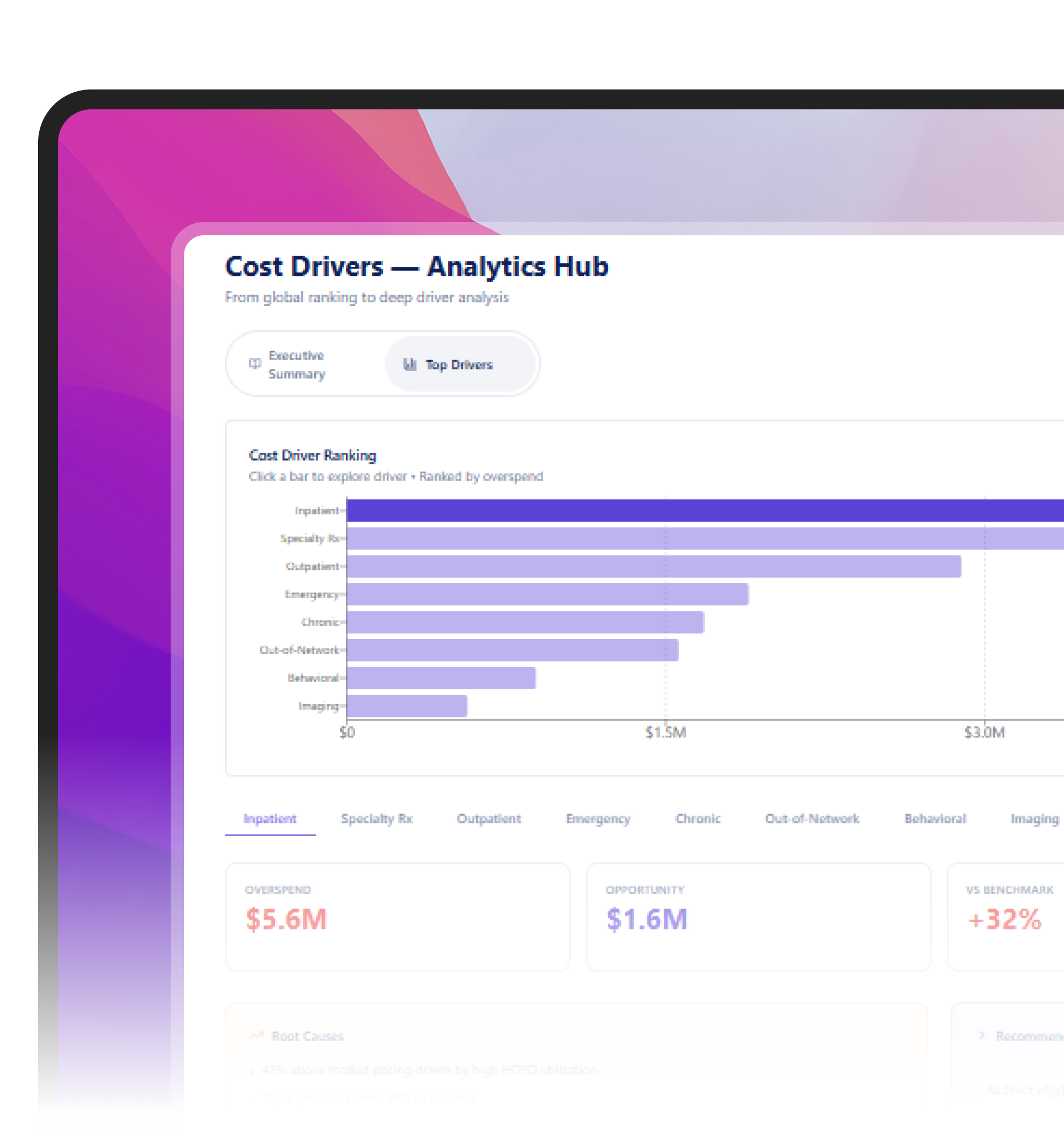
Claims Savings You Can Prove
Reduce up to
10%
of total medical claims spend through pre-pay triage and intervention
Triage
100%
of claims without adding analyst headcount
Loss Ratio
~4%
improvement from claims leakage controls
What Sets BenOsphere Apart
Capability
Real-Time Claims Triage
Pre-Payment Leakage Detection
Price Transparency Benchmarking
Claim-Level Intervention
TPA Workflow Integration
Underwriting Risk Signals
Employer Claims Intelligence
BenOsphere
HealthEdge
GradientAI
Springbuk
Built on National Price Transparency Data
Uses payer and hospital pricing to validate claims in real time.



























































Your Questions, Answered
Still have some questions? Don’t worry. Take a look at our FAQ below.
Does this replace our TPA or existing workflows?
How is this different from post-pay audits or reports?
Will this slow claim payments or member experience?
How do you prove savings and stay fiduciary-safe?
What underwriting signals come from claims triage?
To: price variance + coding anomalies + site-of-care shifts + emerging claims
How does this help Underwriters see risk earlier?
To: High spend = clinical risk + pricing errors + leakage